
Medicare Secondary Payer (MSP) compliance falls on attorneys working on injury claims, workers’ compensation, mass tort actions, and liability settlements. If MSP obligations are not respected, settlements may be delayed; Recovery actions by the Centers for Medicare and Medicaid Services (CMS) against attorney-client relationships may occur; Civil monetary penalties may be assessed to an attorney; and Double damages could be obtained.
As a result, as CMS becomes more vigorous in its enforcement of its rights as a secondary payer, it is imperative that all attorneys understand how MSP regulations apply to their practice, the documentation they will be required to submit, and how to ensure that they are in compliance with those requirements before entering into a settlement with any person or entity.
The following guide provides an attorney-focused resource to answer any questions regarding Medicare Secondary compliance and gives an overview of the MSP’s rules, laws, forms, portals, disability issues, best practices, and the need for proper medical documentation and expert assistance for MSP compliance.
What Is Medicare Secondary Payer (MSP) Compliance?
The MSP legal obligation provides that an entity must ensure that Medicare is not Medicaid is not to be considered a primary payer of medical treatment. Instead, Medicare will only be a secondary payer where another entity is legally responsible for the cost; hence, the entity that has been identified as the primary payer would be the one who is liable for the treatment costs.
- Liability insurance
- Workers’ compensation insurance
- No-fault insurance
- Self-insured entities
For the attorney, complying with the MSP requires the identification of clients on Medicare, the submission of claims to the Medicare system, the reimbursement of conditional payments to Medicare, and protecting Medicare’s future interests when entering into a settlement or obtaining a court verdict for his/her client.
Medicare Secondary Payer Rules, Requirements & Law
Understanding Medicare Secondary Payer obligations requires clarity on its rules, statutory requirements, and governing laws.
Medicare Secondary Payer Rules
Key Medicare Secondary Payer rules attorneys must follow include:
- Medicare does not pay first when another payer is responsible
- Conditional payments made by Medicare must be reimbursed
- Settlements, judgments, and awards must consider Medicare’s interests
- Failure to comply may trigger recovery actions or penalties
These rules apply across personal injury, product liability, medical malpractice, and workers’ compensation cases.
Medicare Secondary Payer Requirements
The core Medicare Secondary Payer compliance requirements for attorneys include:
- Identifying Medicare beneficiaries early
- Reporting claims through proper CMS channels
- Reviewing medical records to isolate injury-related treatment
- Calculating conditional payments accurately
- Ensuring settlement-ready MSP documentation
This is where medical records review for MSP compliance and MSP-focused medical chronology services become indispensable.
Medicare Secondary Payer Law
The Medicare Secondary Payer statute is codified under: 42 U.S.C. § 1395y(b)
This law grants Medicare the right to recover payments when another payer is responsible and allows CMS to seek double damages if reimbursement obligations are ignored. Attorneys, insurers, and self-insured entities can all be held liable under Medicare Secondary Payer law.
Medicare Secondary Payer Forms & Documentation
Accurate and Medicare-compliant documentation is the backbone of Medicare Secondary compliance.
Medicare Secondary Payer (MSP) Form
The Medicare Secondary Payer Form collects information about:
- Accident or injury details
- Other insurance coverage
- Liability or workers’ compensation involvement
Attorneys must ensure this form is completed accurately to prevent claim denials or recovery delays.
Medicare Secondary Payer Fact Sheet
The Medicare Secondary Payer Fact Sheet helps attorneys understand:
- When Medicare is primary vs secondary
- Reporting responsibilities
- Recovery rights and timelines
Using this fact sheet alongside Medicare-compliant medical documentation strengthens compliance and audit readiness.
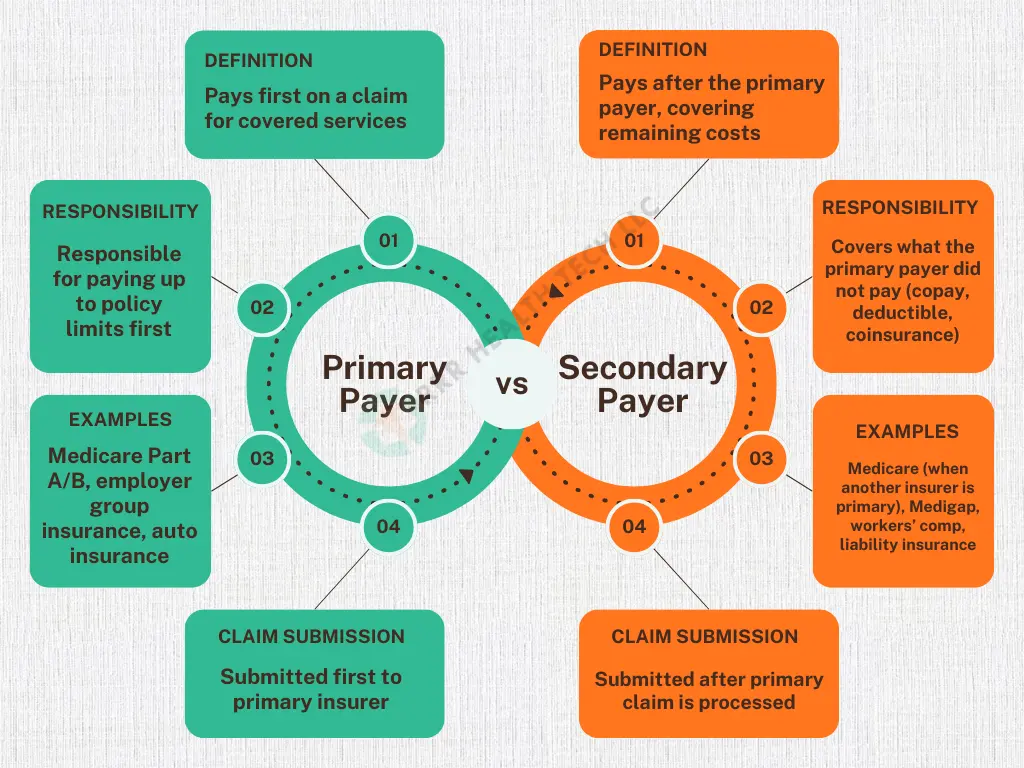
What is the difference between primary payer and secondary payer in Medicare?
Medicare Secondary Payer Portal (MSP Portal): Purpose & Attorney Use
The Medicare Secondary Portal (MSP Portal) allows attorneys and authorized representatives to:
- View conditional payment summaries
- Dispute unrelated charges
- Monitor reimbursement status
- Communicate with CMS efficiently
Proper use of the MSP Portal reduces delays and supports settlement closure with confidence.
Medicare Secondary Payer Disability Rules & Considerations
Special Medicare Secondary Payer rules apply when claimants qualify for Medicare due to disability rather than age.
Key considerations include:
- 24-month SSDI waiting period
- Ongoing future medical treatment
- Medicare Set-Aside (MSA) considerations
- Long-term exposure for CMS recovery
Attorneys must carefully analyze medical timelines using MSP-focused medical chronology services to avoid overlooking Medicare’s future interests.
Medicaid Secondary Payer Act vs Medicare MSP: Key Differences
Although often confused, the Medicaid Secondary Payer Act differs significantly from Medicare Secondary Payer obligations.
| Aspect | Medicare Secondary Payer | Medicaid Secondary Payer |
| Governing Law | Federal (42 U.S.C. §1395y) | Federal + State Laws |
| Recovery Scope | Past & future medicals | Past medicals only |
| Enforcement | CMS (Federal) | State Medicaid Agencies |
| Documentation | CMS forms, MSP Portal | State-specific liens |
| Penalties | Double damages possible | State lien enforcement |
Understanding these differences is essential to avoid compliance errors, especially in dual-eligible cases.
Why Medical Documentation Is Critical for MSP Compliance
Successful Medicare Secondary Payer compliance depends on:
- Accurate injury-related treatment identification
- Clear timelines of care
- Exclusion of unrelated medical conditions
- Proper linkage between injury and billed services
This is achieved through:
- medical records review for MSP compliance
- Medicare-compliant medical documentation
- expert MSP compliance support for attorneys
Without these, attorneys risk inflated conditional payment demands and delayed settlements.
Frequently Asked Questions (FAQs)
How do I know if my Medicare is a secondary payer?
If there is another insurance company, like liability, workers comp, or no-fault, that is responsible (by law) for the payment of medical costs for an injury or illness, then Medicare becomes the secondary payer.
How do you bill Medicare when it is a secondary payer?
The secondary payer will not make a conditional payment unless the primary payer has not paid within a reasonable time. If a conditional payment is made, that amount has to be recovered from the primary payer according to the Medicare Secondary Payer regulation.
What are the cases when Medicare is the secondary payer?
Medicare acts as a secondary payer in cases involving:
- Personal injury settlements
- Workers’ compensation claims
- Product liability lawsuits
- Medical malpractice cases
- No-fault or liability insurance coverage
Conclusion
Medicare Secondary Payer compliance and policies is no longer an option for attorneys, it is a requirement both legally and financially. It is critical for each attorney to manage the entire process of understanding the Medicare Secondary Payer laws, documents, and portals, as well as the reimbursement requirements to be able to achieve the correct outcome for their clients.
Attorneys can experience faster case resolutions, reduced exposure to potential litigation, and improved overall case results by using the expertise of MSP compliance professionals, by utilizing MSP-focused medical chronology services, and by creating settlement-ready MSP documentation.
Expert Legal Support for Medicare Secondary Payer Cases
Navigating Medicare Secondary Payer compliance doesn’t have to slow your cases down. Our team provides:
- Comprehensive medical records review for MSP compliance
- Accurate Medicare-compliant medical documentation
- Dispute-ready conditional payment analysis
- Attorney-focused MSP compliance support
Contact us today to strengthen your Medicare Secondary Payer strategy, protect your settlements, and stay fully compliant with CMS requirements.


