
Accurate and compliant Workers’ Compensation Bill Review is crucial for law firms, insurers, employers, and third-party administrators aiming to control claim costs and ensure fair provider reimbursement. With rising healthcare expenses and increasingly complex billing standards, a strong Workers’ Compensation Bill Review strategy can significantly reduce overpayments, prevent fraud, and ensure compliance with both federal and state guidelines—especially in jurisdictions like Compensation Bill Review California, where regulatory oversight is strict.
This guide breaks down the essential phases of Compensation Bill Review, shares best practices, and explains how Expert Medical Opinion services support the accuracy and defensibility of every review.
What Is Workers Compensation Bill Review?
Compensation Bill Review is the systematic evaluation of medical bills submitted by treatment providers for injured workers. The process ensures that charges align with:
- State fee schedules
- Treatment guidelines
- Appropriate medical necessity
- Correct billing codes
- Applicable legal standards
Attorneys often reference a Workers’ Compensation Bill Review example when examining disputed bills during litigation or settlement discussions.
Using Expert Medical Opinion services can significantly enhance defensibility by validating the medical necessity of specific procedures, especially when facing disputes involving costly surgeries, complex therapies, or contested treatment decisions.
Workers’ Compensation Medical Bill Review Process Explained
Workers’ compensation medical bill review is an important first step in the claims processing workflow for Workers’ Compensation (WC) claims to ensure that submitted claims are compliant with the Workers’ Compensation laws and regulations, along with the applicable fee schedule for every state.
A thorough WC claim bill review will assist in identifying improper billing, overbilling, and provide the necessary documentation to support accurate reimbursement. The following is a breakdown of all key steps in the Workers’ Compensation bill review process.
Medical bill intake & coding validation
The first step of the Workers’ Compensation bill review process is medical bill intake and coding validation. Medical bills are received and then reviewed for proper coding (the collection of codes used to identify a procedure), the correct treatment and procedure descriptions, and the correct routing of invoices. Medical bill intake and coding validation provides an important foundation to verify that the diagnosis, procedures, and services match the corresponding standard medical codes (CPT and ICD).
Compliance with workers’ comp fee schedules
The requirement to comply with the fee schedule for medical providers for workers’ compensation claims will help ensure that the charges of medical providers are within state-specific reimbursement limits set forth by each state. There are, therefore, state-established reimbursement limits for all procedures, services, and treatments provided for WC claims. Medical bill reviews help verify that all submitted charges comply with the fee schedule and prevent a medical provider from receiving an excessive payment.
Identifying overbilling & duplicate charges
Auditors must carefully scrutinize bills to identify excessive charges, repeat times for services, and erroneously charged procedures, as part of a medical bill audit. Overcharging can be caused by a mistake during billing or intentional misrepresentation; likewise, multiple submissions for one service usually result in multiple charges being issued.
By identifying and correcting these types of discrepancies, insurers, employers, and providers can avoid incurring massive expenses due to unnecessary overcharges, as well as establish accountability for providing accurate claims. This technique also allows insurers/employers to accurately manage their workers’ compensation claim costs.
Workers’ Compensation Medical Bill Review for Accurate Cost Control
The process of workers’ compensation (WC) medical bill review entails reviewing medical bills associated with work-related injuries to confirm proper billing, compliance with WC, and determine the cost-effectiveness of services. Medical coding standards will be used when verifying bills against inaudible charges and/or services that are either charged twice or used inappropriately. Additionally, medical bill review will guarantee that all charges are in accordance with their respective states specific WC fee schedules.
WC medical bill review will provide benefits to multiple user groups including, but not limited to, attorneys, insurance companies, and the employer. Attorneys will utilize WC medical bill review to bolster their legal proceedings, insurance companies will be able to monitor the costs associated with claims, and employers will minimize their financial liability and maintain compliance by virtue of WC medical bill review.
Key Steps in the Workers’ Compensation Bill Review Process
Insurance carriers, employers, and law firms rely on standardized steps to streamline the Workers’ Compensation Bill Review workflow. Below is a detailed breakdown of the phases involved.
Step 1: Intake and Verification (Workers’ Compensation Bill Review Foundation)
At this stage, adjusters gather all bills, supporting medical records, and claim information. Verification includes:
- Date of injury
- Provider credentials
- Relationship to compensable body parts
- Duplicate billing detection
This step may also include referencing a Workers’ Compensation Bill Review PDF or internal guidelines to ensure proper documentation.
Step 2: Fee Schedule Compliance Review
One of the most important components of Workers’ Compensation Bill Review is checking billed charges against state fee schedules. For example, Workers’ Compensation Bill Review California uses a combination of OMFS rules, RBRVS, and state-mandated guidelines.
Reviewers examine:
- CPT/HCPCS code accuracy
- UCR benchmarks
- Application of modifiers
- Facility vs. non-facility rates
Step 3: Medical Necessity Review with Expert Medical Opinion Services
Billing accuracy isn’t enough; attorneys and insurers must determine whether treatments are medically necessary. This is where Expert Medical Opinion services become crucial.
Medical reviews assess:
- Whether treatment aligns with evidence-based guidelines
- Whether prolonged therapies are justified
- Whether surgeries or injections were appropriate
- Whether diagnostic tests were medically necessary
This stage often influences IBR decisions, particularly when disputes arise about excessive or unjustified billing.
Step 4: Application of PPO, Network Discounts, and Policies
Many Workers’ Compensation Bill Review companies apply additional cost-saving measures such as:
- Preferred provider network discounts
- Negotiated reductions
- Policy-based caps
This ensures bills reflect all applicable contractual savings.
Step 5: Final Report, Payment Recommendations & Dispute Preparation
After adjustments, the final review includes:
- Adjusted bill amounts
- Denials with explanations
- Coding corrections
- Documentation for payment
If disputes arise, the claims team may reference:
- Independent Bill Review forms
- Second Bill Review forms
- Carrier-specific appeal documentation
Attorneys often use a Workers’ Compensation Bill Review example to illustrate proper reductions and defend fee schedule adjustments.
Best Practices for Improving the Workers’ Compensation Bill Review Process
Attorneys, insurers, and employers can strengthen their Workers’ Compensation Bill Review process by implementing these strategies:
1. Use Advanced Workers’ Compensation Bill Review Software
Modern workers compensation bill review software improves accuracy through:
- Automated coding validation
- Duplicate bill detection
- Fee schedule updates
- Integrated medical guidelines
This reduces human error and accelerates review timelines.
2. Partner with Reputable Workers’ Compensation Bill Review Companies
Top workers compensation medical bill review companies and workers comp bill review companies provide specialized expertise, updated technology, and accurate analytics. Their experience helps reduce costs and avoid compliance issues.
3. Incorporate Expert Medical Opinion Services into Every Review
Using medical expert’s increases:
- Defensibility during litigation
- Clarity on medical necessity
- Successful IBR decisions
- Strategic insight for complex or high-dollar claims
4. Maintain Clear Documentation for Disputes
Complete and organized documentation supports better legal outcomes, especially for:
- Provider disputes
- Independent Bill Review requests
- Appeals related to surgical care or diagnostic procedures
Bill Review Companies vs Bill Review Software in Workers Compensation
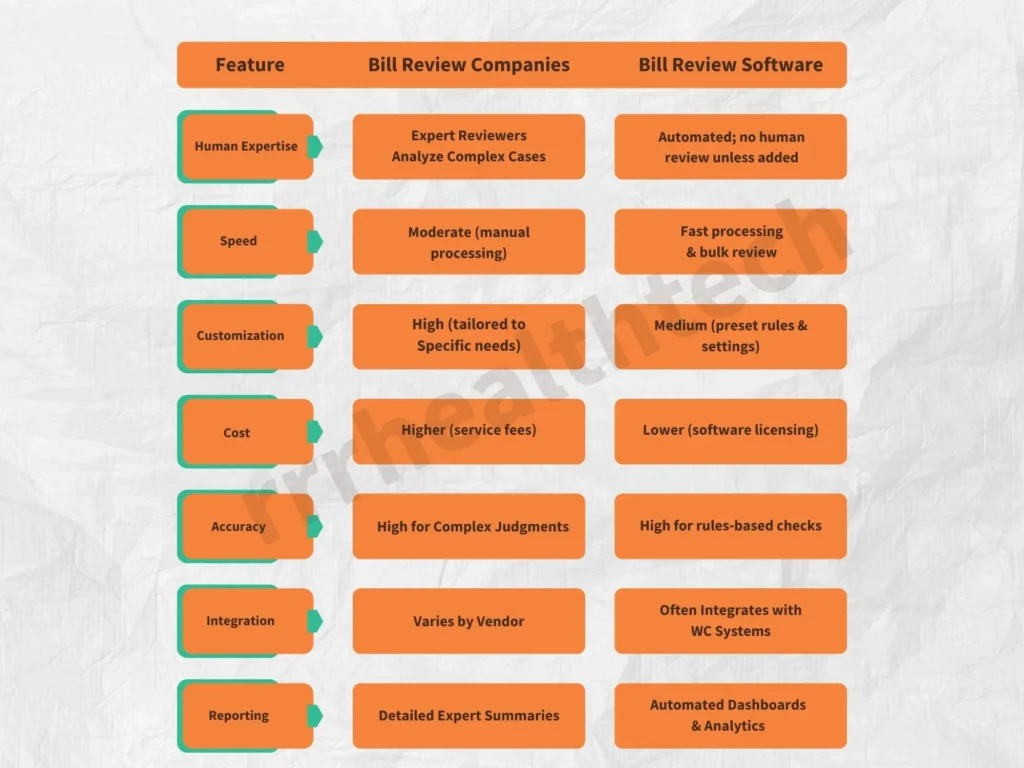
Conclusion
A well-structured Workers’ Compensation Bill Review process protects employers, insurers, and attorneys from excessive costs, billing errors, and compliance risks. With the right technology, expert medical insights, and review partners, you can optimize accuracy, streamline claims, and defend your decisions confidently.
Frequently Asked Questions
What is Workers’ Compensation Bill Review and why is it important?
It is the process of evaluating medical bills submitted for work-related injuries to ensure compliance, prevent overpayment, and validate medical necessity. It helps reduce costs and improves claim accuracy.
What are the key steps involved in the Workers’ Compensation Bill Review process?
The process includes verification, fee schedule review, medical necessity evaluation, applying network discounts, and generating final payment recommendations.
How can employers and insurers improve their Compensation Bill Review practices?
Using modern review software, partnering with experienced review companies, leveraging Expert Medical Opinion services, and maintaining strong documentation all enhance efficiency and compliance.
Need medical-legal expertise or support with Workers’ Compensation Bill Review? Contact us today for reliable, attorney-focused services that strengthen your claims strategy.


